Written: May 2007
What is rosacea?
With a subtle onset and a combination of symptoms that makes early diagnosis tricky, there’s a lot still to be discovered about the red face of rosacea. But, while the exact cause is still being researched, we do know that it is a chronic (persistent and long-lasting) inflammatory vascular disorder that affects blood vessels, nerves and connective tissues, primarily in the facial area.
The blood vessels within areas of rosacea skin are hyper-responsive to a wide range of stimuli, meaning that they dilate and flood with blood more frequently than those of normal skin. This initially results in recurrent red blushing, then the more often you flush, the more damage is done to your blood vessels and the more serious the visible effects will become.
Symptoms & stages of development
Rosacea can appear slightly differently in different people, but primary features include erythema (flushing), papules, pustules, and telangiectasia (visibly dilated blood vessels or ‘spider veins’). Other signs include a burning or stinging sensation, dryness, plaques of red inflammation and swelling or pitting due to oedema (accumulation of lymph fluid). Symptoms may also go through periods of remission and exacerbation.
Left to its own devices, rosacea is a progressive disorder. The International Dermal Institute recognises three progressive stages of the disorder:
Pre-rosacea
People prone to frequent, transient bouts of blushing are placed in this category. Although the redness fades as soon as the stimulus (e.g. heat, embarrassment, exercise or a skincare product) is removed and no visible damage remains, this innocent-looking flush is considered the first cardinal sign of rosacea as the blood vessels reveal their tendency to dilate abnormally.
Stage 1 (early rosacea)
This mild stage of rosacea can be recognised when redness stimulated by a trigger remains for half an hour or more after the cause disappears. In some cases, the flush can take days to dissipate. Though some might begin to itch, burn and appear less tolerant to skincare products, rosacea research specialist Dr Geoffrey Nase notes that “many rosacea sufferers [at this stage] also report that their facial skin has a healthy-looking glow.” Ironically, this ‘healthy’ rosy glow is really a red flag of distress.
Stage 2 (moderate rosacea)
Facial flushing becomes more frequent and intense now, with ruddiness lasting for days or weeks. Some areas of skin can appear chapped or ‘sunburned’ and may also feel swollen, hot and uncomfortable. Inflammatory papules and pustules may appear and, in most cases, prominent areas of telangiectasia will be visible where flushing is worst.
Stage 3 (advanced rosacea)
This stage is characterised by intense flushing and inflammation, burning sensations and, as blood vessels are structurally damaged and lymph accumulates, an irregular ‘spongy’ skin texture, swelling and facial pain. Inflamed crops of papules and pustules can arise and sebaceous glands may appear enlarged on the cheeks and nose. In the most severe cases, facial contours can distort and rhinophyma, a bulbous enlargement of the nose, can emerge. While rhinophyma is most commonly suffered by men, women can also experience similar distortion on the cheeks or chin. If left untreated, rhinophyma can develop into nflammatory nodules on the face and ears.
Ocular rosacea
Rosacea of the eye area may also appear during the moderate to severe stages of facial rosacea. Signs include a persistent burning and ‘gritty’ feeling in the eye or swollen eyelids that feature small inflamed bumps. Eyes may also be watery, bloodshot or sensitive to light and have some blurred vision. The most frequent symptoms, which may never progress, include lid inflammation, crusting and irregularity of the eyelid margin.
Acne vs. rosacea
The presence of redness, oiliness and inflamed pustules and papules often leads to confusion between acne and facial rosacea, but the distinction is important as acne treatments can irritate and exacerbate rosacea. “Acne and rosacea can co-exist,” explains dermatologist Dr Catherine Reid, “but that’s rare as the times of onset are usually different for each.”

Who is susceptible?
Women are far more likely to develop rosacea than men, though when men do develop the disorder, they tend to suffer more severely. Fair people of Northern European and Celtic descent are also more at risk of rosacea and, though the precise genetic link has not yet been identified, the disorder is thought to have a hereditary link.
Could you have rosacea?
Only a dermatologist or GP can diagnose rosacea for sure. “It’s difficult to recognise in the early stages because some of the symptoms might look like other things, like sun damage,” explains Dr Reid. “People often only come to me when the symptoms become a cosmetic issue, like when the spots [papules and pustules] or telangiectasia appear.”
So how do you recognise rosacea early enough to avoid stage two signs? “If you notice you’re flushing a lot, it seems to last for ages and someone in your family has similar signs or has been diagnosed with rosacea, it’s worth going to the GP or dermatologist to have it checked out,” advises Emma Hobson from the International Dermal Institute.
Managing rosacea
There’s no absolute cure, but the good news is that, with proper care, the progression and appearance of rosacea can be controlled.
Dealing with triggers
The key to controlling rosacea is identifying the triggers of your flare-ups and learning to avoid them. Keep a record of which foods, conditions and products provoke your rosacea and then steer as clear of them as you can.
Diet – Although alcohol can be a tripwire for rosacea symptoms, it is not a cause of rosacea (as often believed) and is no more a culprit than caffeine, spicy foods or a bowl of hot soup. Histamine-producing foods including tomato, yoghurts and cheeses, citrus fruits, avocadoes, canned fish, vinegars, and fermented beverages can also fan the flames. Ask your doctor about the Elimination Diet if you’re having trouble pinpointing problem foods.
Exercise – Vigorous and cardiovascular exercise can often be a major trigger for rosacea skin as hyper-responsive vessels dilate to accommodate blood rushes. Light exercise such as yoga, lots of water and cool compresses can help stop you getting flustered.
Stress and fatigue – Feeling frantic, unrested or even just embarrassed stimulates the sympathetic nervous system and causes facial blood vessels to dilate. Leading a balanced lifestyle and taking care of yourself can help tone it down.
Sun exposure & the elements – Extremes of heat and cold are common triggers and the sun can spark a wildfire of inflammation. Limiting your exposure to the elements and sunscreen (fragrance-free is best) is important.
Menopause – Hot ‘flushes’ from hormonal fluctuations can cause flare-ups during menopause.
Skincare & cosmetics – Though the International Dermal Institute says cosmetic products are not a major overall trigger of rosacea (in comparison to other factors), some products can cause the skin to sting or flush. Ingredients to avoid include artificial fragrances and alcohol, witch hazel, menthol, peppermint and eucalyptus as well as chemicals found in acne treatments, chemical sunscreens and topical steroids. Harsh products, heat-based treatments and vigorous exfoliants are also likely to provoke a red reaction.
The International Dermal Institute suggests rosacea sufferers seek out soothing ingredients like aloe, allantoin, arnica, oats, chamomile, green tea, mallow, liquorice and red clover.
It can be tough to find beauty products developed specifically for rosacea, but, as long as they don’t feature your known triggers, fragrance-free formulas designed for very sensitive skin can help.
Try:
Dermalogia Daily Microfoliant ($75) is a gentle rice bran-based exfoliant.
Cosmedicine Medimorphosis Exfoliator ($65) contains non-scratchy silicone spheres that gently remove dead surface debris but melt upon contact with the rest of the skin.
Avene Extremely Gentle Cleanser ($30.40) is designed for intolerant faces. It’s rich in soothing thermal water and free from fragrance.
Cetaphil Gentle Skin Cleanser (from $6.50) is a soap-free, pH balanced formula for sensitive skin.
Avene Diroseal ($31.45) has been formulated to gently correct and conceal flushes connected to rosacea. It has a light green tint to help counteract redness.
Clinique CX Redness Relief Cream ($160) is a 100 per cent fragrance-free blend of soothing botanicals and lipids to help comfort and smooth reactive skin.
Dermalogica Sheer Tint Redness Relief ($75.50) features ingredients including oat extract, green tea and liquorice to calm redness. Also contains non-chemical SPF15 protection plus green-tinted minerals to neutralise redness.
Cosmedicine Hydra Healer ($120) contains allantion as well as other deeply moisturising ingredients to provide plumping and hydration benefits without causing irritation.
When using any products on flare-prone skin, Hobson highlights the importance of “the less rule”:
• Less product – Use fewer products, reduce the steps in your routine and apply smaller quantities.
• Less time spent stimulating your skin with your fingers and products.
• Less heat –take short, warm showers, cleanse with tepid water and avoid steam or heat-based treatments.
• Less friction – avoid rubbing and scrubbing your skin with hands or washcloths.
Treatments
By avoiding triggers and using non-irritating products, some people with mild rosacea can prevent the disorder escalating. But those with moderate to more advanced symptoms should check in with a GP or dermatologist.
“Two common treatments that can really help control symptoms include antibiotic tetracycline, which is taken orally, and metronidazole, which is a topical antibiotic that you can apply in a gel or a cream form,” explains Dr Reid. Courses of treatment usually involve both oral antibiotics and topical therapies at first, followed by ongoing topical maintenance.
Lasers or surgery may also be useful for dealing with the more permanent and disfiguring symptoms. “Vascular lasers are very effective for treating telangiectasia,” she says. “And lasers can also be used to pare back the skin of a bulbous nose.”
Emma Hobson champions manual lymphatic drainage for managing the spongy accumulation of lymph (fluid) which may occur in moderate stage rosacea. “It’s not like a deep massage and doesn’t cause friction; it’s more of a gentle ‘pushing’ action where the therapist manually helps the skin do what rosacea stops it from doing naturally. It’s very relaxing and, done every two to three weeks, it can really help improve and maintain skin texture,” she says.
Unfortunately, control over symptoms is all doctors can do for rosacea sufferers at the moment. “But there is hope”, highlights Hobson. “Right now, we don’t understand the causality of rosacea so we don’t have a cure – but there is a lot of work being done on it,” she says. “There is so much research dedicated to it that I’m confident the cure will come. The future is bright.”
– Tracey Withers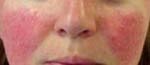




Thanks BH for another informative article.